Around the globe, billions face a critical challenge: the growing gap between healthcare demand and clinical availability. While financial hurdles persist, the ongoing shortage of medical professionals adds a layer of complexity that mere funding cannot resolve. In this scenario, medical artificial intelligence is stepping up as a crucial factor, providing solutions to bridge this gap while waiting for future generations of trained healthcare workers to emerge.
Advanced technological solutions enable healthcare providers to extend their reach into underserved areas, effectively enhancing physician capabilities through digital tools that were once inaccessible. These innovations do more than streamline processes; they play a pivotal role in making healthcare financially viable for families caught in the uncertainty of health-related expenses versus their economic stability.
The influence of AI on global health accessibility is manifested in frontline clinics and through interoperable health devices and telemedicine systems. Rather than acting as replacements for clinicians, these systems efficiently manage data analysis and reduce administrative burdens, allowing healthcare providers to offer high-quality care to a larger number of patients with improved accuracy.

Global Healthcare Affordability and Workforce Shortage Quick Facts
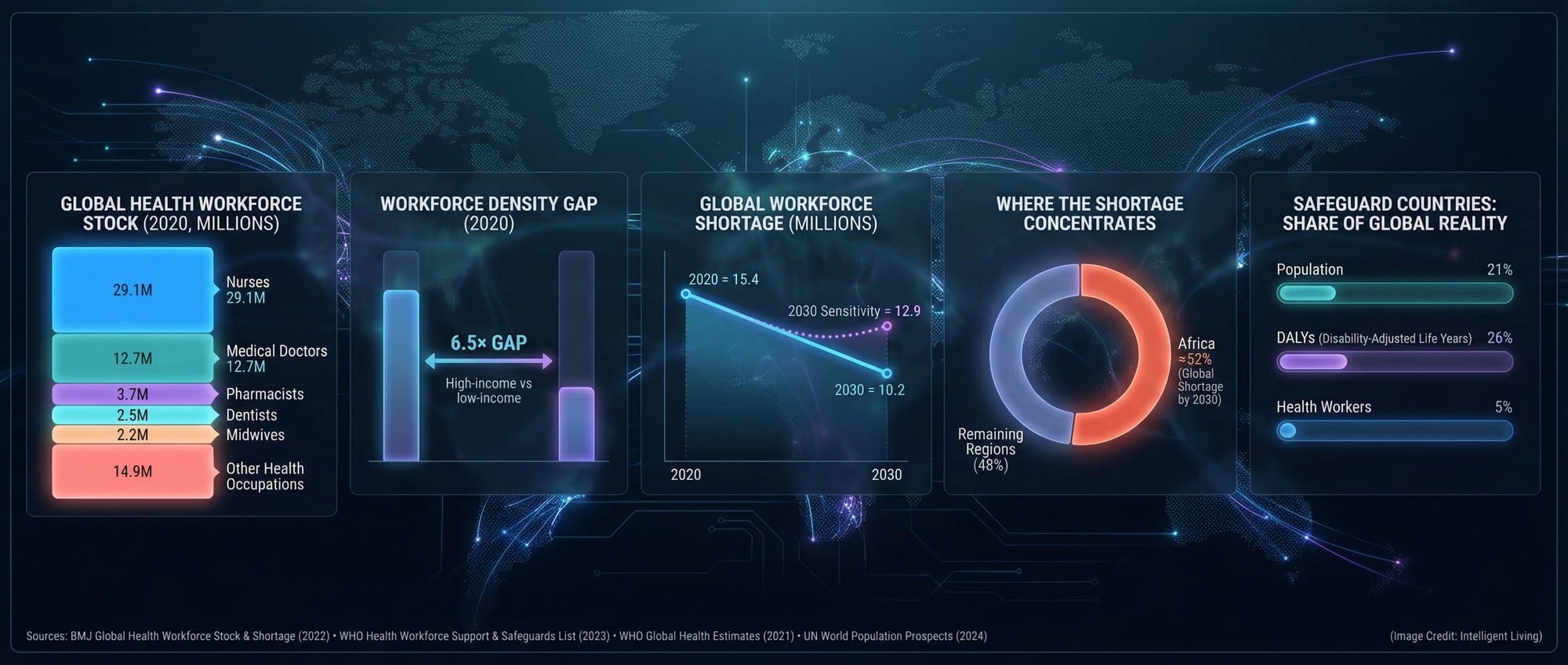
Addressing the Global Physician Shortage through Clinical Capacity Expansion
The Real Crisis is Not Just Cost; It’s Capacity
Many experts frame the issue of healthcare affordability solely in monetary terms; however, the underlying challenge is clinical capacity. Access to care remains limited due to:
- Clinicians being unavailable in optimal locations.
- Services not being accessible at appropriate times.
- Existing healthcare staff struggling under administrative burdens.
An analysis of global healthcare worker distribution suggests that, in 2020, there were approximately 65.1 million health professionals worldwide, including 12.7 million medical doctors. The report highlights a striking 6.5-fold gap in workforce density between high-income and low-income countries, jeopardizing healthcare access in many regions. This shortage poses a significant threat to the goals of universal health coverage, especially in areas identified by the WHO.
Time is also a crucial factor in capacity. Clinician schedules are often consumed by:
- Repetitive documentation and coding tasks.
- Administrative oversight and data entry activities.
- Fragmented digital systems that lack interoperability.
Transitioning public health systems towards digital care ensures clinicians can focus on patient interaction rather than clerical responsibilities. When clinician time becomes scarce, costs naturally rise, making access to care even more challenging.
The Capacity Multiplier: How AI Expands Care Without Adding Doctors
AI-driven clinical decision support systems empower frontline healthcare workers to deliver care that adheres more closely to evidence-based guidelines. The WHO SMART Guidelines initiative aims to convert global clinical recommendations into interoperable digital formats, reduce software development costs, and ensure consistent decision support across different regions.
Imagine the possibilities: a nurse or community health worker equipped with structured digital guidance can effectively manage complex cases. This paradigm shift allows healthcare providers to offer evidence-based care in areas where specialists are scarce. Instead of needing specialist input for every decision, AI-assisted triage can handle routine situations, enabling healthcare systems to prioritize high-risk cases that require immediate human attention. In various regions, advanced practice nurses in primary care demonstrate how clear scope and protocols allow clinician teams to serve more patients.
In rural clinics, for instance, a mid-level provider using structured digital workflows can identify warning signs earlier and escalate them efficiently. This does not replace physicians; it enables them to concentrate on more complex cases, ensuring routine care proceeds without delays.
By broadening effective clinical reach, AI functions as a capacity multiplier, enabling timely care for more individuals even without a substantial increase in the number of physicians.

Cost-Effective Diagnostic Screening With High-Performance AI Software
TB Screening: Chest X-Rays, CAD Software, and Earlier Detection
Diagnostic imaging offers perhaps the most compelling evidence of how AI supports affordability in practical applications. By efficiently processing large volumes of data, these tools enable healthcare facilities to uphold high standards of care while accommodating growing patient loads. The global standards for tuberculosis detection advocate for the use of chest radiography and computer-aided detection software to identify TB earlier in at-risk populations. In locations with limited radiology capabilities, this technology can significantly enhance screening without requiring a radiologist to interpret each initial image.
Diabetic Retinopathy: Cost-Effective Vision Protection
Research from Kerala shows that diabetic retinopathy screening programs are much more affordable than late-stage treatments. The Government of Kerala’s 2019 pilot program indicated a cost per quality-adjusted life year (QALY) of approximately INR 22,000. Another study on cost-effective vision screening in rural settings similarly concluded that AI-supported screening is cost-effective when compared to no screening at all.
On-Device Ultrasound: Maternal Care Without Reliable Connectivity
AI-assisted obstetric ultrasound technology demonstrates excellent results even in low-resource environments. One mobile-compatible system functions entirely without internet, achieving accurate gestational age estimates. This study confirmed high reliability in automated fetal positioning and age assessment without the need for expert interpretation. Hardware advancements align with this software progress, including automated scanning via tomographic ultrasound robots.
Why Early Detection Can Cut Household Health Costs
A parent taking their child for screening may not visually grasp the algorithmic processes at work. However, they do experience the advantages of faster waiting times and more accurate results. When families can rely on these swift results, they are less likely to defer care due to financial constraints.
Scalable screening initiatives play a vital role in mitigating the catastrophic expenses associated with late-stage diseases. This rationale also supports the creation of tools like thermal bra inserts that monitor breast health for early intervention.
Why Follow-Up Determines Whether Screening Lowers Costs
Screening processes alone do not lead to reduced costs without timely follow-up care. The combination of remote monitoring and predictive analytics is essential for ensuring patients receive appropriate interventions when necessary.
Evidence Snapshot: Conversational AI Monitoring and Risk Prediction
A prospective pilot study evaluated remote heart failure monitoring using conversational tools, reporting minimal nurse workload and encouraging positive outcomes. More than just heart failure monitoring, machine learning models built on non-invasive data have shown enhanced predictive capabilities in clinical environments. These remote monitoring systems precisely identify risks for heart failure hospitalization more effectively than traditional methods.
Turning Monitoring into Early Action Before Readmissions
When patients are monitored in their own homes, early warning signs can trigger timely interventions before conditions worsen. Regular risk assessment serves as a key mechanism for preventing avoidable hospital admissions.
Wearables and Recovery Monitoring that Make Follow-Up Practical
Wearable technology can facilitate effective follow-up routines. Examples include wearable sensors for continuous heart rate monitoring and innovations like thermoelectric sensors for health tracking. Battery-free microchips also offer consistent monitoring capabilities, making frequent follow-ups achievable. Moreover, smart bandages can enhance the tracking of wound healing, reducing the risks associated with late-stage complications.

Eliminating Administrative Drag to Maximize Clinical Workforce Efficiency
The Paperwork Tax: How AI Gives Clinicians Time Back
The often-overlooked burden of administrative tasks remains a significant driver of rising healthcare costs, diverting hours away from crucial patient interactions. Tasks like documentation, coding, and electronic health record management consume substantial time for clinicians.
Extensive studies have indicated that using ambient AI solutions can effectively decrease clinician burnout by alleviating documentation burdens. When clinical staff spend less time on paperwork, they can redirect considerable energy back into direct patient care.
In a bustling urban clinic, for example, this could translate into additional appointment slots each week. Administrative bottlenecks often obstruct patient flow even before they step into the consultation room. Thus, automated clinical intake and scheduling become crucial cost-saving mechanisms alongside clinical AI deployment. This pattern is evident in specialty clinics as well, such as where digitizing telemental health documentation workflows proves beneficial.
Symptom Checkers and Digital Triage: What the Evidence Shows
Consumer-oriented AI tools, like symptom checkers and digital triage systems, are often touted as an initial access point. They direct patients to suitable care levels and potentially reduce unnecessary visits. However, evidence assessing AI symptom checker performance shows marked variability in triage accuracy.
Key insights from an audit on symptom checker reliability highlight:
- Correct diagnoses were listed first only about one-third of the time.
- Appropriate triage guidance was given in just over half of cases.
- Accuracy rates vary significantly across different standardized assessments.
These results emphasize that while digital solutions uniquely enhance convenience, they need rigorous human oversight to ensure patient safety.
Safety Tradeoffs: False Reassurance Versus Over-Triage
For a parent searching “AI symptom checker for child fever” online, the balance between reassurance and the risk of false negatives is crucial. Similarly, over-triage can lead to increased unnecessary utilization and expenses.
Triage Under Pressure: Urgent Care Workflows
In urgent care settings where timing is critical, integrating AI triage with health record systems illustrates that establishing accuracy benchmarks and escalation pathways is vital.
Governance Guardrails: Transparency, Equity, and Human Oversight
Recent ethical guidelines for health-based AI systems stress the importance of transparency, accountability, and fairness.
The safe deployment of AI tools requires strict validation frameworks to ensure reliable operation. Clear escalation routes are essential for effectively managing uncertainty and safety limits. Current initiatives prioritize empowering clinical teams through conversational AI within regular workflows.
Mental Health and Community Access: Validation Still Matters
Digital engagement can broaden access, particularly in expanding mental health services via community-centered telehealth initiatives. Nonetheless, validation remains crucial for biometric data in digital mental health assessments conducted through personal devices.
While affordability gains from digital triage are attainable, they hinge on prioritizing patient safety and regulatory oversight.

Scaling Universal Health Coverage Through Interoperable Digital Infrastructure
Achieving UHC Requires More than Funding—It Needs a Completely Reimagined Operating System for Care
Achieving universal health coverage involves more than just financing reforms; it requires a robust interoperable digital infrastructure that facilitates evidence-based decision-making, effective referral systems, and ethical data management. A global roadmap for equitable digital health outlines interoperability, governance, and human capacity as cornerstones for scalability.
The UHC global monitoring report provides detailed regional insights and technical appendices and regional data tables. These resources indicate where progress is stagnating and highlight areas most affected by financial hardships.
Constructing infrastructure requires a strategic framework for future digital healthcare. This roadmap positions interoperability and governance as prerequisites for scaling care without exacerbating existing inequalities. Affordability increases when care delivery is standardized, data flows seamlessly, and prompt detection is linked to structured follow-up. Thus, AI becomes integral to a new operational framework for healthcare delivery.
A Practical Playbook: What Countries and Health Systems Can Do Next
- Focus on proven clinical applications: Implement technology where the evidence is strongest, such as tuberculosis CAD screening and digital chronic disease management models.
- Integrate the screen-to-follow-up loop: Ensure every diagnostic program is paired with a scalable monitoring and intervention system to safeguard patient well-being.
- Reduce administrative overhead: Utilize ambient documentation technologies in high-demand environments to expand effective capacity.
- Establish governance frameworks: Adhere to WHO guidelines for ethical AI deployment.
- Evaluate crucial metrics: Measure cost per case detected, hospitalizations prevented, and clinician time saved to gauge overall effectiveness.
Policymakers assessing the potential of AI may discover that targeted implementations yield significant benefits without necessitating large-scale changes. Operational tools simplify interactions through streamlined patient communication systems. Additionally, virtual nursing for remote bedside support in hospital settings enhances patient care directly.

Empowering Global Health through Intelligent Capacity Expansion
The ongoing shortage of physicians presents a structural crisis that cannot be remedied by conventional recruitment strategies alone. Artificial intelligence offers a unique pathway to transform healthcare delivery, maximizing the effectiveness of limited clinician time. Achieving universal health coverage necessitates shifting from slow, cumbersome processes to agile, data-informed systems that prioritize care across diverse regions.
Our advancement in this transformation relies on a global commitment to safety and equity, underpinned by constant human oversight. By employing AI to prevent costly hospital readmissions and enhance early detection, we can foster a more resilient health ecosystem. Harmonizing technological power with human insight is essential to ensure accessibility for all.
Common Questions About AI in Modern Healthcare
Does AI Aim to Replace Human Doctors in Shortage Areas?
No, these tools serve as capacity enhancers. They handle routine tasks and data management, allowing physicians to devote their attention to more complex cases requiring human expertise.
How Exactly Does AI Support Healthcare Affordability?
AI reduces costs by facilitating early illness detection and minimizing administrative inefficiencies, helping prevent expensive late-stage health crises and maximizing clinical productivity.
Can Patients Trust The Accuracy of AI-Based Triage?
While accuracy can vary, clinical validation and clear escalation processes are essential. These systems are designed to assist rather than replace, professional oversight.
What Role Does AI Play in Reducing Hospital Readmissions?
Predictive analytics and remote monitoring can identify early signs of health declines, enabling care teams to intervene before emergencies arise.
What Are The Core Governance Requirements for Responsible AI?
Governments need to prioritize transparency, data privacy, and ethical frameworks. Continuous oversight is necessary to ensure that AI tools promote equity rather than exacerbate existing disparities.